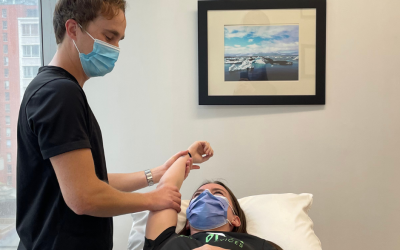
Trigger Point Dry Needling
Dry Needling. Maybe you’ve heard of it, maybe you haven’t! Those who have usually fall into one of these three categories:
1) They’ve tried acupuncture before and aren’t sure how dry needling differs.
2) They know someone who’s tried it and refer to it as the ‘Buckley’s’ of treatment interventions – it tastes awful (can be uncomfortable)…… but it works!
3) They’re terrified of needles and wouldn’t even dream of giving this a try.
So what is Dry Needling really? How does it work and who may benefit from this treatment modality? Keep reading to learn more!
What is Trigger Point Dry Needling?
Trigger Point Dry Needling is a treatment technique dating back to the 1970s and is used by highly trained health-care providers around the world. It is performed by inserting a thin monofilament needle into the skin and underlying muscular tissue where a myofascial trigger point has been identified. It can be used to treat myofascial pain syndromes with the goal of reducing pain and optimizing tolerance and effectiveness of targeted therapeutic exercise.
A myofascial trigger point is defined as “a hyperirritable spot, usually within a taut band of a skeletal muscle or in the muscle’s fascia, that is painful when compressed and can give rise to characteristic referred pain.” An active trigger point can cause local or referred pain, muscle weakness, and autonomic phenomena. Whereas latent trigger points are only painful when stimulated, but can still alter muscle patterning and range of motion. Taut bands in muscular tissue are a normal occurrence in response to sustained postures, lack of loading or exceeding the capacity of a muscle. When taut bands arise, the tissue releases a chemical called acetylcholine which triggers hyperactivity (contraction) of the muscle. If a taut band becomes chronic or persistent this prolonged hyperactivity of the muscle leads to pain due to tissue hypoxia (reduced blood flow to that area of the muscle).
Trigger Point Dry Needling has been shown to have immediate effects on pain reduction, range of motion and muscle tone in myofascial pain syndromes by stimulating what is referred to as a “local twitch response”. This is when the muscle being treated has an involuntary contraction, leading to an alteration in the length and tension of the muscle. It is also thought that dry needling can reduce pain associated with hypoxia by stimulating local vasodilation and subsequently increasing the amount of oxygenated blood in the muscle.
What is the difference between acupuncture and dry needling?
While dry needling and acupuncture both involve the insertion of needles into the skin, this is the only similarity between the two modalities. Acupuncture is based around Traditional Chinese Medicine (TCM) and refers to inserting needles along ‘Meridians’ – energy pathways throughout the body. The theory is that pain, injury or illness can be the result of interruption in the flow of energy along a meridian and that acupuncture can restore this. Acupuncture has also been adapted under the lens of “Western Medicine” where it is used to stimulate nerves and muscles. It is thought to increase blood flow and stimulate the nervous system in order to treat musculoskeletal pain. In contrast, dry needling is the insertion of needles into both the skin and muscle tissue of muscles with myofascial trigger points in order to relieve the presence of pain and muscle tension.
What to expect?
During a Dry Needling session your practitioner will identify the muscle(s) which may have trigger points and could benefit from treatment. Once these muscles are identified they will sanitize their hands and the area being treated and begin. During the treatment you may experience the muscle(s) twitch, pressure and/or a deep ache in the muscle – this is normal! Some patients may feel a mild ache in the muscle for a short time after treatment that can be compared to the feeling you may experience in your shoulder after an immunization. This feeling is typically eased with movement of the area that was treated (ie. light cycling or walking if the lower body is treated).
NOTE: Dry Needling is a treatment modality that is best used as an adjunct treatment technique in order to optimize your ability to complete the therapeutic exercise or apply any other recommendations necessary to make long-term change. Most of the time, Dry Needling alone is not an effective way of treating. Without changing the underlying reason for the development of myofascial trigger points you may end up requiring ongoing treatment. (DO YOUR EXERCISES!!!)
If you have any questions about whether Trigger Point Dry Needling may be an appropriate treatment technique for you – lets chat!
– Kristen Blair, Registered Physiotherapist

References:
Dunning J, Butts R, Mourad F, Young I, Flannagan S, Perreault T. Dry needling: a literature review with implications for clinical practice guidelines. Phys Ther Rev. 2014 Aug;19(4):252-265. doi: 10.1179/108331913X13844245102034. PMID: 25143704; PMCID: PMC4117383.
Jan Dommerholt, Orlando Mayoral del Moral & Christian Gröbli (2006) Trigger Point Dry Needling, Journal of Manual & Manipulative Therapy, 14:4, 70E-87E, DOI: 10.1179/jmt.2006.14.4.70E
Institute of Medicine (US) Committee on Pain, Disability, and Chronic Illness Behavior; Osterweis M, Kleinman A, Mechanic D, editors.
Washington (DC): National Academies Press (US); 1987.
Bron, C., Dommerholt, J.D. Etiology of Myofascial Trigger Points. Curr Pain Headache Rep 16, 439–444 (2012). https://doi.org/10.1007/s11916-012-0289-4